[et_pb_section bb_built=”1″ _builder_version=”3.0.100″ custom_padding=”20px|0px|22px|0px”][et_pb_row custom_padding=”20px|0px|0px|0px” _builder_version=”3.0.100″ border_width_all=”1px” box_shadow_style=”preset1″ box_shadow_blur=”36px”][et_pb_column type=”4_4″][et_pb_text admin_label=”News – August 2011″ _builder_version=”3.17.6″ background_color=”#ffffff” animation_style=”fade” custom_margin=”|||” custom_padding=”|20px|20px|20px”]
Welcome to Niche Medical’s Customer Newsletter – August 2011
This newsletter is designed to inform our customers of the latest information on our products and services.
We highly value your input and feedback and encourage you to send all feedback and comments to Craig Abud by simply replying to this email.
If for any reason you do not wish to receive this newsletter in the future, simply click on the SafeUnsubscribe button at the bottom of this newsletter.
Please feel free to pass this newsletter onto those who may find it valuable. There is a forward email icon located at the bottom of this newsletter.
Craig Abud, Niche Medical
Proven Lifetime Stability for the EasyOne Spirometer
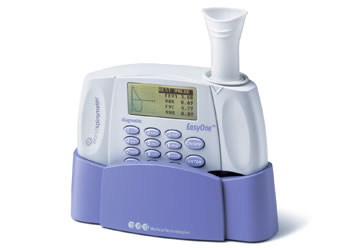
A recently published study by Skloot et al (Respiratory Care – July 2010) has shown that the EasyOne spirometer retained inhalation and exhalation volume accuracy of better than 3% for at least 4 years. (1).
The authors concluded that the acceptability and repeatability of patient efforts should be the primary focus of quality-assurance programs with spirometers that have been demonstrated to remain accurate for long periods.
In fact the EasyOne spirometers used in this intervention (Lung Function in Rescue Workers at the World Trade Center after 7 Years) had been in use since August 2002 so therefore these EasyOne spirometers have maintained their calibration for over 7 years which is essentially the lifetime of the instrument. (2).
This study supports the findings of previous studies which demonstrated the stability of the EasyOne spirometer over periods of three to six months. (3,4).
The manufacturer of the EasyOne spirometer (ndd Medical Technologies) issues a Certificate of Stability guaranteeing that every instrument is life time stable and needs no calibration checks what so ever.*
1. Four-Year Calibration Stability of the EasyOne Portable Spirometer – Skloot et al –
Respir Care 2010;55(7): 873- 877.
2. Lung Function in Rescue Workers at the World Trade Center after 7 Years – Aldrich et al – n engl j med 362;14 April 8, 2010.
3. Stability of the EasyOne ultrasonic spirometer for use in general practice – Walters et al – Respirology (2006) 11, 306-310.
4. The Long-Term Stability of Portable Spirometers Used in a Multinational Study of the Prevalence of Chronic Obstructive Pulmonary Disease – Padilla et al – Respir Care – October 2006 VOL 51 NO 10 1167.
* Some clinical studies and / or other applicable guidelines do call for frequent calibration or calibration checks. This is required for spirometers not following the ndd measurement principle i.e. for spirometers that have not been shown to be stable over the long term. In the case of the EasyOne spirometer you can follow such guidelines calling for calibration check procedures by choosing “Check Calibration” which you will find in the main menu of the EasyOne spirometer. Note that ndd instruments cannot and do not need to be calibrated.
Bedfont Smokerlyzer CO Monitors

Niche Medical is pleased to annouce that we are now the exclusive suppliers of the Bedfont range of Smokerlyzer Breath CO (Carbon Monoxide) Monitors in Australia.
What is a Smokerlyzer?
Smokerlyzers are a range of breath CO (Carbon Monoxide) monitors and testers which measure the small amounts of CO in the exhaled breath. The more a person smokes, the higher their CO reading will be.
The reading is given in ppm, which is the number of CO molecules in a million parts of air. The ppm reading can also tell you how much CO is in the blood (the %COHb reading). %COHb is the percentage of red blood cells carrying CO instead of oxygen.
The amount of CO in an unborn baby’s blood is referred to as %FCOHb (percentage of foetal carboxyhaemoglobin). Some of the Smokerlyzer range can analyse %FCOHb as an incentive to stop smoking and complies with the new NICE guidelines for smoking in pregnancy.
Why monitor CO?
CO testing is a quick, non-invasive and cost-effective means of validating the smoking status of a significant number of clients. Smoking is the single greatest avoidable risk factor for lung cancer.
Carbon monoxide monitors offer tobacco treatment specialists an independent clinical tool which provides valuable evidence in identifying, educating, assessing and treating tobacco-dependent patients.
Monitoring patients’ CO levels helps to work out their level of nicotine dependence: the more they smoke, the higher their reading will be, indicating a higher dependence on nicotine.
There are four Smokerlyzers in the Bedfont range as follows:
- Micro+ Smokerlyzer (One CO monitor for all your testing needs).
- piCO & Smokerlyzer (a firm favourite for motivation, validation and education).
- babyCOmpact Smokerlyzer (Stop Smoking support for mothers to be).
- COmpact Smokerlyzer – (The most cost effective smokerlyzer in the world).
NIOX MINO – FeNO Measurement
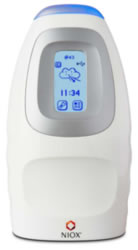
Introducing the NIOX MINO from Aerocrine:
- Calibration and Maintenance-free FeNO device.
- All FeNO-values quality assured.
- Individualised data management for the Practice and the patient.
- Prepared for direct communication to patient Electronic Medical Record (EMR).
- NIOX MINO Visual Incentive.
- Cable (USB) or wireless (Bluetooth) connection to a PC makes it possible to follow the procedure on the PC screen.
Inflammation measurement with NIOX MINO offers personalised asthma management that can dramatically improve the treatment and care of your patients.
Several underlying diseases can present symptoms similar to asthma. Therefore, a correct diagnosis relies on establishing whether or not the patient is characterised by allergic airway inflammation.
Until recently, diagnostic devices have not been able to convey a complete clinical overview and clearly identify the underlying cause of the symptoms. Consequently, patients that are not suffering from asthma have received unnecessary or inadequate treatment. 1.
Patients with asthma symptoms due to allergic inflammation will respond favourably to inhaled corticosteroids, while those who are suffering from other airway disorders may not. 2,3.
Measuring exhaled NO (FeNO ) helps to eliminate the uncertainties and discrepancies that contribute to asthma morbidity and mortality, including incorrect diagnosis and poor adherence to treatment.
Nitric Oxide (NO) – a marker of inflammation. Monitoring asthma symptoms is important , but correct interpretation of the underlying inflammation determines the therapy. Measuring exhaled NO provides an immediate answer to three critical questions:
- Which patients with non-specific or multiple respiratory symptoms have allergic airway inflammation?
- Is the patient adhering and responding to the prescribed therapy?
- Has there been a change in allergen exposure?
NIOX MINO reveals:
- Allergic inflammation of the airways. 4.
- Whether the patient is compliant with anti-inflammatory therapy. 6.
- Changes in allergen exposure. 6.
Additional features:
- Instrument memory of up to 3000 measurements which can easily be transferred to the NIOX MINO Data Management Program on a PC.
- Inhalation of NO-free air. NIOX MINO removes ambient NO, which ensures accuracy and follows the recommendations by ATS/ERS.
- Infection control with a disposable bacterial and viral filter prevents contamination of the device and between patients.
- Builds on the ATS/ERS Recommendations
- Nasal FeNO Research Application
Nasal Research Application With the NIOX MINO Nasal Application nasal FeNO concentration can be measured in gas aspirated from a nostril using passive sampling.
References
1. Aaron SD, Vandemheen KL, Boulet LP, McIvor RA, Fitzgerald JM, Hernandez P, Lemiere C, S Harma S, Field SK, Alvarez GG, Dales RE, Doucette S, Fergusson D; Canadian Respiratory Clinical Research Consortium, Overdiagnosis of asthma in obese and nonobese adults. CMAJ. 2008. 18;179(11):p. 1121-31.
2. Berry, M.A., D.E. Shaw, R.H. Green, C.E. Brightling, A.J. Wardlaw, and I.D. Pavord, The use of exhaled nitric oxide concentration to identify eosinophilic airway inflammation: an observational study in adults with asthma. Clin Exp Allergy, 2005. 35(9): p. 1175-9.
3. Smith, A.D., J.O. Cowan, K.P. Brassett, S. Filsell, C. McLachlan, G. Monti-Sheehan, G . Peter Herbison, and D. Robin Taylor, Exhaled nitric oxide: a predictor of steroid response. Am J Respir Crit Care Med, 2005. 172(4): p. 453-9
4. Sandrini A, Taylor DR, Thomas PS, Yates DH, Fractional exhaled nitric oxide in asthma: an update. Respirology. 2010;15(1): p: 57-70.
5. S Zefler, S.J., H. Mitchell, C.A. Sorkness, P.J. Gergen, G.T. O’Connor, W.J. Morgan, M. Kattan, A. Pongracic, S.J. Teach, G.R. Bloomberg, P.A. Eggleston, R.S. Gruchalla, C.M. Kercsmar, A.H. Liu, J.J. Wildfire, M.D. Curry, and W.W. Busse, Management of asthma based on exhaled nitric oxide in addition to guideline-based treatment for inner-city adolescents and young adults: a randomised controlled trial. Lancet, 2008.372(9643): p. 1065-72.
6. Vahlkvist, S., M. Sinding, K. Skamstrup, and H. Bisgaard, Daily home measurements of exhaled nitric oxide in asthmatic children during natural birch pollen exposure. J Allergy Clin Immunol, 2006. 117(6): p. 1272-6.
The Lung Flute – Diagnostic and Therapeutic
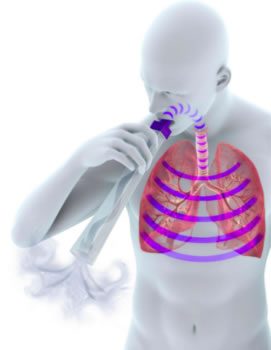
Introducing the dual-indicated Diagnostic and Therapeutic Lung Flute.
The DIAGNOSTIC Lung Flute is designed to be an alternative to hypertonic saline for sputum induction in respiratory diseases such as Cystic Fibrosis, Pneumonia, Lung Cancer, Tuberculosis and Asthma.
Lung Flute features include:
- Simple hand-held disposable device
- Low pressure operation
A low frequency acoustic wave is generated at the mouth by exhaling through a mouthpiece over a laminar surface (Reed) inside the Lung Flute. The resulting low frequency acoustic wave that is produced travels retrograde into the lower airways and lung parenchyma and increases mucociliary clearance.
Patients expel air with the force required to blow out a single candle. 20 repetitions of a single two breath pattern are performed with the device to complete a diagnostic session.
Clinical Results for Sputum Induction in Tuberculosis
Background and Objective: The Lung Flute is a small self-powered audio device that generates sound waves, which vibrate in tracheobronchial secretions. This was a preliminary trial to evaluate the usefulness of the Lung Flute for sputum sampling in patients suspected of pulmonary tuberculosis (TB).
Methods: Thirty-four patients who were not expectorating sputum, but for whom sputum examination was required for the differential diagnosis of TB or other diseases, were enrolled in the study. Patients were instructed to blow out fast and hard through the Lung Flute and to repeat this for a total 20 sets of two blows each.
Results: Using the Lung Flute, sputum samples were collected within 10 or 20 minutes from 30 of 34 patients (88%). The device permitted a rapid diagnosis of TB in seven of 15 confirmed TB cases. In three patients acidfast bacillus smears were positive. In four patients acid-fast bacillus smears were negative, but PCR tests for TB were positive. Hyperventilation-related symptoms occurred in three patients.
Conclusions: The application of the Lung Flute may represent a promising technique for the rapid diagnosis of Pulmonary Tuberculosis.
The Lung Flute is a safe, effective, convenient and rapid method of sputum induction.
The THERAPEUTIC Lung Flute is indicated for Positive Expiratory Pressure (PEP) Therapy and is clinically proven to be an effective method for Mucociliary Clearance.
Lung Flute features include:
- Simple hand-held device
- Low pressure operation
- Replaceable reeds
Clinical Results for Mucociliary Clearance in COPD
In a recent clinical trial conducted at The WNY VA Medical Center by the University at Buffalo, School of Medicine, the performance of the Therapeutic Lung Flute was compared to that of the Acapella device.
In this 8-week trial, changes in 24-hour sputum collection was the primary endpoint. Secondary endpoints were changes in spirometry and quality of life. Changes in the quality of life questionnaires were noted for both devices. A larger reduction in symptoms was seen with the Lung Flute with the CCQ.
However, the differences between the two devices were not statistically significant. Disease related health status is an important efficacy end point in COPD.
The Lung Flute did show larger improvements in health status than the other device as measured by the SGRQ, though the difference did not reach statistical significance.
The Lung Flute presents a safe, effective, convenient and rapid method of secretion mobilisation.
EasyOne Pro LabSystem
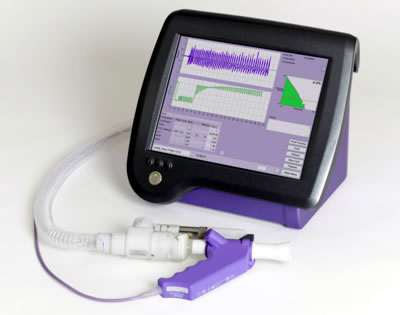
Introducing the new EasyOne Pro LabSystem which builds on the EasyOne Pro DLCO System with the addtion of the Multi Breath Washout Module for the determination of FRC (Functional Residual Capacity), LCI (Lung Clearance Index) and derived parameters.
In addition to the basic EasyOne Pro this instrument provides more detailed information about lung volumes and airways disturbance.
An additional gas input for the Multi-Breath Washout test gas is provided; normally oxygen, but alternatively gas mixtures with SF6 (Sulfur Hexafluoride) or Helium maybe used. Oxygen as commonly available in central gas supplies (wall outlets) is suitable, facilitating convenient bed side testing.
The FRC valve / washout gas supply unit is mounted on the left hand side wall of the housing, camouflaged by the cover in EasyOne Pro colour. Physical dimensions change therefore insignificantly from the standard EasyOne Pro unit. To prevent connection error, the inlet diameter of the MBW test gas is different from the one for the DLCO test gas.
The software in the EasyWare Pro LabSystem contains an additional module for MBW analysis which facilitates a smooth and simple MWB FRC procedure in a neat, precise and smart way.
The EasyOne Pro LabSystem provides a number of additional parameters including the Lung Clearance Index (LCI) which is not available in common body box systems.
Measured Parameters:
- CEV (Cumulative Expired Volume)
- FRC (Functional Residual Capacity)
- LCI (Lung Clearance Index)
- MR0, MR1, MR2 (Moment Ratios)
- RV (Residual Volume)
- TLC (Total Lung Capacity)
The EasyOne Pro LabSystem has been developed based on the ATS guidelines as referred to in:
Am. J. Respir. Crit. Care Med. Vol 175. pp 1304-1345, 2007 (Page 1328 et sqq.)
Why choose the EasyOne Pro LabSystem?
- Minimal patient cooperation and minimal system deadspace (makes testing easier for paediatric and obstructive patients)
- No valve resistance
- Very simple, calibration free test procedure makes it easy for the operator and the patient
- EasyOne Pro FRC can be operated with common O2 (hospital wall outlet)
- Portability for all bedside and POCT applications
LiteAire Spacer – Tested in Humans

The LiteAire Disposable Cardboard Spacer offers proven clinical efficacy and convenience with minimal storage requirements and an environmentally friendly alternative to large rigid plastic spacers.
In a poster presentation from researchers at the Princess Margaret Hospital for Children at the recent TSANZ / ANZSRS Conference in Perth the efficacy (Bronchodilator Response) of the LiteAire spacer was shown to be clinically equivalent to that of a Large Volume Spacer when tested in children aged 6-18 years with doctor diagnosed asthma.
In addition, a study published in the Journal of Emergency Medicine in 2009 demonstrated that the LiteAire Disposable Spacer is clinically equivalent to nebuliser therapy in the treatment of acute adult asthma in the Emergency Department setting.
These are both very important findings for the LiteAire Spacer given that the recently introduced semi-disposable spacers have never been tested in-vivo.
Rather these semi-disposable spacers have only been tested in the laboratory setting where the results do not necessarily translate into the clinical setting.
So when it comes to choosing a spacer for your healthcare facility why not choose the LiteAire spacer which delivers proven results in real patients.
Have you got the latest software for your EasyOne Spirometer?

The EasyWare and Easy on-PC software are upgraded 2-3 times per year and you can download the latest software free of charge from the manufacturer’s (ndd Medical Technologies) website at
http://www.ndd.ch/Downloads/software.aspx
These software downloads are executable files so if you work in a Hospital or a Government agency please make sure you have an IT person present to download and install the software as these type of files require administrator permission.
Once you have downloaded and installed the latest EasyWare software you should then connect your EasyOne spirometer to your computer and run the EasyWare software as this will also update the internal software in your EasyOne Spirometer.
If you require any assistance please telephone us on 1300 136 855.
Click on this link to download the latest EasyWare or Easy on-PC software
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
